Acute Rheumatic Fever
Infections, Inflammatory, Pediatrics
First 5 Minutes
There is no gold standard laboratory test.
Acute rheumatic fever can rarely present as heart failure or stroke due to combination of cardiomyopathy and valvulopathy.
- Treat heart failure.
- Consider acute rheumatic fever as cause of the heart failure or stroke
Context
- Acute rheumatic fever (ARF) is an autoimmune inflammatory reaction secondary to group A streptococcal (GAS) pharyngitis. ARF, especially if recurrent, may lead to the development of rheumatic heart disease (RHD).
- RHD has significant morbidity and mortality, and is the most common acquired heart disease
- RHD can lead to heart failure, stroke, or death
- RHD is preventable through the detection and treatment of GAS pharyngitis insofar as avoiding episodes of ARF.
- GAS pharyngitis occurs primarily in children between the ages of 5 and 15 in the winter and early spring.
- When to suspect ARF:
- Children with polyarthritis or new onset cardiac murmurs
- Less commonly, ARF may present with chorea or skin manifestations
- Most common among children aged 10-14, followed by ages 5-9
- Rheumatic heart disease secondary to acute rheumatic fever remains a serious problem in low and middle income countries and among marginalized populations around the world.
Diagnostic Process
- Diagnosis is clinical and based on the presence of various major and/or minor features. The features required to diagnose ARF depend on whether the presentation is new or recurrent.
- Patients are divided into low-risk (incidence of ARF ≤2 per 100,000 children or RHD ≤1 per 1,000 total population) and moderate- and high-risk populations.
- High risk includes: living in ARF endemic area, indigenous heritage, past history of ARF or RHD, overcrowding or low socioeconomic status, family or household history of ARF. A 2015 study found the incidence of ARF among First Nation children in NW Ontario was 21.3 per 100,000.
- Initial ARF → evidence of preceding GAS infection and 2 MAJOR manifestations OR 1 MAJOR and 2 MINOR manifestations
- Recurrent ARF → evidence of preceding GAS infection and 2 MAJOR manifestations OR 1 MAJOR and 2 MINOR manifestations OR 3 MINOR manifestations
- Major Criteria:
- Low-Risk Pop: clinical and/or subclinical carditis (including echocardiographic valvulitis), polyarthritis, chorea, erythema marginatum, and subcutaneous nodules
- Moderate- to High-Risk Pop: clinical and/or subclinical carditis, monoarthritis/polyarthritis/polyarthralgia (polyarthralgia after exclusion of other causes), chorea, erythema marginatum, and subcutaneous nodules
- Minor Criteria:
- Low-Risk Pop: polyarthralgia, fever >38.5 degrees, ESR ≥60mm in first hour and/or CRP ≥3.0mg/dL, and prolonged PR interval (after accounting for age variability unless carditis is a major criterion)
- Moderate- to High-Risk Pop: monoarthralgia, fever >38.5 degrees, ESR ≥30mm in first hour and/or CRP ≥3.0mg/dL, and prolonged PR interval (after accounting for age variability unless carditis is a major criterion)
- Summary of ARF Clinical Findings:
- Carditis (50-70%) and arthritis of large joints (35-66%) are the most common manifestations.
- Sydenham chorea presents as involuntary and non-stereotypical movements of the trunk or extremities.
- Arthritis involves the large joints and lasts approximately 4-weeks
- Erythema marginatum (<6%) presents as an erythematous, evanescent, non-pruritic, and serpiginous rash that typically presents on the trunk and proximal extremities.
- Subcutaneous nodules (0-10%) present on extensor surfaces.
- GAS Features: Sudden onset sore throat, pain with swallowing, fever, scarlet fever rash, headache, red and swollen uvula, tender anterior lymphadenopathy, patient 5 – 15 years old, tonsillopharyngeal erythema and exudates, nausea, vomiting, and abdominal pain.
- Investigations:
- Echocardiography with Doppler in all confirmed and suspected cases of ARF (Class 1, Level B)
- Anti-Streptolysin O titers or other streptococcal antibodies (e.g. anti-DNAse B) can help bolster diagnosis of GAS pharyngitis (Class 1, Level B)
- GAS throat culture or positive rapid GAS antigen test in the case of high pre-test probability for GAS pharyngitis (Class 1, Level B)
- CBC and CRP/ ESR
- ECG and Chest x-ray
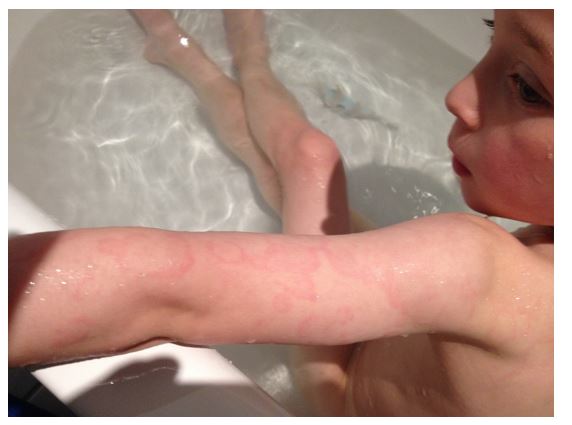
Figure 1: Erythema Marginatum. https://commons.wikimedia.org/wiki/File:Erythema_marginatum.jpg. Image accessed from Wikimedia Commons.
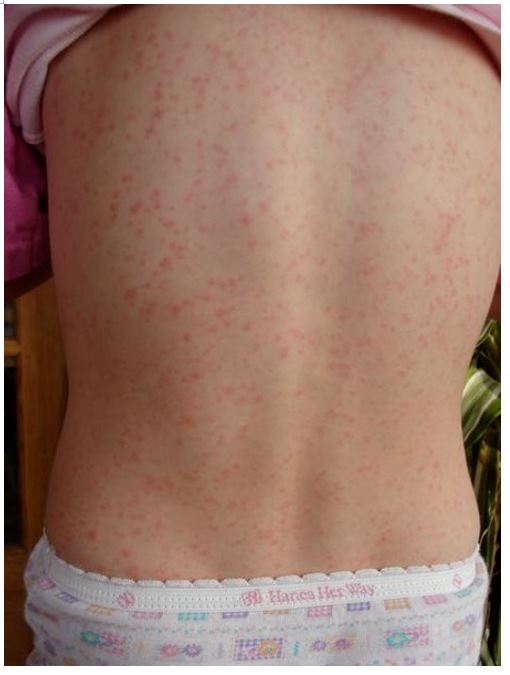
Figure 2: Scarlet Fever Rash. https://commons.wikimedia.org/wiki/File:Scarlet_fever_2.jpg
Recommended Treatment
Treatment is divided into primary treatment, secondary prevention and symptomatic treatment
- Treat inciting GAS infection
- Symptomatic treatment (e.g. arthritis, carditis, and chorea)
- Prevent progression to chronic RHD
- GAS infection should be treated regardless of presence of pharyngitis
- Single IM dose of Penicillin G benzathine is preferred – avoids noncompliance and is first dose in secondary prophylaxis.
- Benzathine penicillin G 600,000 IU for children and 1.2M IU for adolescents and those ≥27kg.
- Refer to pedmed.org
- Single IM dose of Penicillin G benzathine is preferred – avoids noncompliance and is first dose in secondary prophylaxis.
OR
-
- 10 days of penicillin V 250mg BID for children and 500mg BID for adolescents or those ≥27kg.
- Patients with carditis causing heart failure or rheumatic heart disease will require additional cardiac treatment which will not be discussed in this clinical summary.
Secondary prevention
- benzathine penicillin G every 4 weeks in doses of 600,000IU for children and 1.2M IU for adolescents and those ≥27kg is used.
- If oral is preferred, patients can take penicillin V 0.5g daily for children and 1g daily for adolescents and those ≥27kg.
- Duration = 5-10 years = consultant decision.
Symptomatic Treatment
- Arthritis
- Acetaminophen until the diagnosis is established, then treatment with naproxen 10-20mg/kg/day BID can be initiated.
- Carditis
- Restrict physical activity for 4-6 weeks
- Mild to moderate:
- ASA 80-100 mg/kg PO daily
- Moderate to severe
- Consider prednisone 2 mg/kg PO daily x 2 weeks then taper off
- Lack of evidence that corticosteroids are more effective than ASA
- No evidence for IVIG changing disease outcome
- Consider prednisone 2 mg/kg PO daily x 2 weeks then taper off
- Aspirin and corticosteroids have been shown not to demonstrate improvement in cardiac outcomes at one year after diagnosis.
- Chorea treatment is supportive
Surgery for valvopathy – aortic regurgitation initially then progresses to stenosis
Criteria For Hospital Admission
Most patients with acute rheumatic fever are admitted to hospital to facilitate diagnostic work-up, initiate treatment, and provide education to the patient and the family.
Criteria For Transfer To Another Facility
Patients would require transfer to a capable centre facilitate the above investigations (e.g. echocardiogram, blood tests), and in-patient pediatric care.
Criteria For Close Observation And/or Consult
Patients with acute rheumatic fever, and especially those with carditis require referral to cardiology for ongoing management and serial echocardiography.
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
Information presented in this clinical summary is primarily taken from the American Heart Association and is endorsed by the American Academy of Pediatrics. The quality of evidence varies throughout the review, but is consistently rated as “Class I” and “Grade A or B” (data derived from multiple high-quality clinical trials or single high-quality randomized/nonrandomized studies).
Related Information
OTHER RELEVANT INFORMATION
Reference List
Webb R, Grant C, Harnden A. Acute Rheumatic Fever. BMJ. 2015; 35:1-8. doi: 10.1136/bmj.h3443
Gerber MA, Baltimore RS, Eaton CB, Gewitz M, Rowley AH, Shulman ST, Taubert KA. Prevention of Rheumatic Fever and Diagnosis and Treatment of Acute Streptococcal Pharyngitis. Circulation. 2009; 119: 1541-1551. DOI: 10.1161/CIRCULATIONAHA.109.191959
Gordon J, Kirlew M, Schreiber Y, Saginur R, Bocking N, Blakelock B, Haavaldsrud M, Kennedy C, Farrel T, Douglas L, Kelly L. Acute rheumatic fever in First Nations communities in northwestern Ontario. Canadian Family Physician. 2015; 61: 881-886. PMID: 26759842; PMCID: PMC4607335.
Gewitz MH, Baltimore RS, Tani LY, Sable CA, Shulman ST, Carapetis J, Remenyi B, Taubert KA, Bolger AF, Beerman L, Mayosi BM, Beaton A, Pandian NG, Kaplan EL. 2015. Revision of the Jones Criteria for the diagnosis of acute rheumatic fever in the era of Doppler echocardiography. Circul. 131(20):1806-1818.
RESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Jan 02, 2024
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.