Necrotizing Fasciitis – Diagnosis
Infections
Context
- Necrotizing fasciitis is a rare but life/limb threatening disease and is a true surgical emergency.
- There are about 100 cases annually in Canada (1/350,000).
- There are 3 types:
- Type I: Polymicrobial: Typical risk factors include diabetes, peripheral vascular disease (PVD), and advanced age. Can occur in urogenital region (Fournier’s gangrene).
- Type II: Group A streptococcal necrotizing fasciitis (“flesh-eating disease”). Few or no risk factors.
- Type III: Clostridial myonecrosis (gas gangrene). This skeletal muscle infection may be associated with recent surgery or trauma.
Diagnostic Process
- Necrotizing fasciitis is a clinical diagnosis.
- The hallmark is pain out of proportion to findings. The clinician should have a high level of suspicion and low threshold for surgical consultation in cases of severe pain, swelling, and fever. Furthermore, the physician should have a high index of suspicion for patients who present with severe pain in an anatomic area, with no other cause; necrotizing fasciitis may have severe pain as the ONLY symptom early on in the presentation.
- Early necrotizing fasciitis may present with no marks/lesions on the skin, and non-specific symptoms.
- Necrotizing fasciitis may follow minor trauma to the skin or varicella skin infection. A high index of suspicion is essential. Blood tests (elevated WBC, C-Reactive Protein, or CK) are non-specific. Typical labs drawn are CBC, eclectrolytes, BUN, CR (GFR), C Reactive Protein, INR, LFTs and an ECG.
- Presence of bullae or gas in tissue (see images below) is a late finding with the latter usually only seen in Type III necrotizing fasciitis.
- Plain xrays can also be done but have poor sensitivity.
- MRI has reasonable sensitivity for detecting necrotizing fasciitis, but surgical consultation should not be delayed for imaging for suspected necrotizing fasciitis. It is better to refer early, and have it be a false positive!
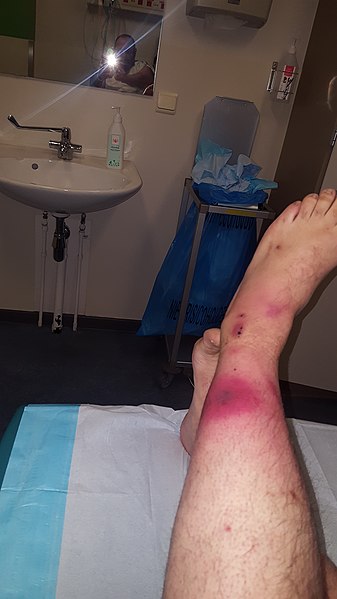
https://commons.wikimedia.org/wiki/File:Early_symptoms_of_NF.jpg
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
Because of the rarity of necrotizing fasciitis, there are few studies to draw on. These are retrospective studies and frequently based on expert opinion.
Related Information
OTHER RELEVANT INFORMATION
Necrotizing Fasciitis (St Paul’s EM Update 2018)
Presenter: Simon Jones, Clinical Instructor, UBC Department of Emergency Medicine
Reference List
Relevant Resources
RELEVANT RESEARCH IN BC
Sepsis and Soft Tissue InfectionsRESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Nov 01, 2022
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.