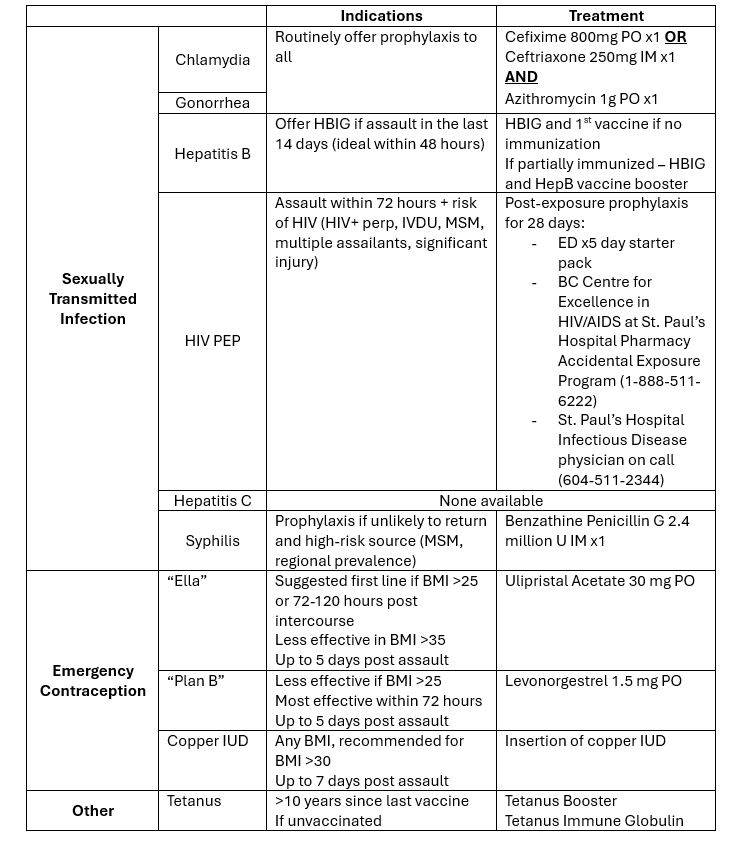
Sexual Assault – Treatment
Equity, Diversity, and Inclusion (EDI), Obstetrics and Gynecology, Special Populations, Trauma
Context
- Sexual assault (SA) is a crime of power and control.
- 1/3 women and 1/6 men will experience a sexual assault in their lifetime.
- 96% of perpetrators are male.
- An approach to sexual assault applies principles of trauma-informed care: safety, trustworthiness, choice, collaboration, empowerment.
- How the patient is treated at the outset (i.e. with compassion, validation and giving them their choice in their care journey) will guide their subsequent course in how they handle the trauma of their assault.
- Medical treatment is different and separate from forensics. Patients should be able to get decent medical care at any ER/UCC/FD office in BC.
- Forensics are nice if we can have it, and only if the patient wants. Forensic care is mostly only offered at specialized sites within each Health Authority. We generally have a bit of time to get forensics, but ideally sooner the better, especially if looking for toxicology.
Context
Emotional and psychosocial care:
- Acknowledge difficulty and courage in seeking care.
- Respond with empathy, belief, and without judgment.“What happened is not your fault.”
- Offer to have support person to accompany patient, if available (patient friend, family, and/or through community organization (see Patient Community Resources section below).
- Identify existing sources of support and coping strategies.
- Consider offering referrals to:
- Mental health services for post-assault counselling.
- Social work.
Criteria For Safe Discharge Home
- Safety plan in place.
- Options for post-assault counselling and social support offered.
- See “Patient Community Resources” section below.
- Social Work.
- Mental Health Services.
- Follow up:
- With family physician (if they have one).
- Lab testing:
- Pregnancy test in 1 month.
- HIV and syphilis in 1 and 3 months.
- Prescriptions for STI prophylaxis if started in ED.
- For ex. HIV PEP for 28 days.
- Completion of Hepatitis B vaccination (if first dose provided during visit).
Criteria for Consult
- Requiring psychiatric stabilization.
- Currently Pregnant and/or at risk of miscarrying.
- Immunocompromised.
- Requires a Copper IUD insertion.
- severe trauma including genital or ABD trauma (eg. Perforated viscus), or strangulation with airway concerns or Loss of consciousness.
Criteria For Transfer To Another Facility
- Transfer to sexual assault service for medical and/or forensic examination within 7 days of the assault (call RACE line, see hospitals with sexual assault services)
- Severe trauma.
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
Summarized from regional protocols. May vary regionally within the province.
Other Resources
Patient Community Resources
- Women Against Violence Against Women (Rape Crisis Line, counselling services, 3rd party reporting, hospital accompaniment in Lower Mainland).
- VictimLink (information and referral services).
- British Columbia Society for Male Survivors of Sexual Abuse (support services for male victims).
- Health Initiative for Men (support and information for gay men).
- Qmunity (counselling, information, referrals, peer support for LGBTQ people).
Recommended Courses
Related Information
Reference List
Relevant Resources
RESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Jul 23, 2020
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.