Inherited Bleeding Disorders
Hematological / Oncological, Infections, Special Populations
First 5 Minutes
FACTOR FIRST CARD: Guidelines for Emergency Management of Hemophilia and Von Willebrand Disease
In Hospital Care of Persons with Inherited Bleeding Disorders (PwIBD)
- PROMPT TRIAGE AND ASSESSMENT. PwIBD should be triaged urgently as delays in administering appropriate therapy, can significantly affect morbidity and mortality.
- DETERMINE THE LOCATION AND SEVERITY OF BLEED. Treatment for a suspected bleeding episode should be based on clinical history, findings could be normal in the early stages.

- POTENTIALLY LIFE THREATENING bleeds to the head, spine, abdomen or pelvis could initially be occult. An Occult hemorrhage that progresses may produce emergent circumstances.
- ASK THE PATIENT if they have a Factor/Treat First Card or if they are followed by the Adult or Pediatric Bleeding Disorder Program of BC/Yukon. This treatment card provides patient specific dosing for major/minor bleeds and contact information for the programs.
- TREAT FIRST > INVESTIGATE LATER. It is recommended that treatment be given BEFORE any diagnostics studies (ie: X-rays, CT scans etc) are performed to evaluate a suspected bleeding problem or injury, especially in the case of head trauma or suspected intracranial hemorrhage. Early treatment can mitigate further bleeding or complications.
Context
Inherited Bleeding Disorders are rare and when an affected person accesses the ER, historically healthcare providers have not always recognized the urgency of providing timely hemostatic interventions and connecting with experts who can help.
- PwIBD do not bleed more at the time of injury/procedure they do however, bleed for a longer duration causing increased risk of infection, poor healing/recovery, anxiety, hospital admissions, and disabilities.
- The BC Bleeding Disorder Programs of BC/Yukon support these patients over the course of their lives.
- PwIBD that are classified as “MILD”, may have an increased risk of poor outcomes or death. The bleed infrequently and are often unsure when to seek help; have limited experience with bleeds; may present late to the ED; often they do not self-infuse; and will need to access hospital setting or clinic for treatment.
Inherited Bleeding Disorder Summary
- FACTOR PRODUCTS are ordered from the hospital Transfusion Medicine Laboratory NOT
- BLOOD CONSENT is required ONLY for plasma derived factor concentrates (ie: Humate P, FEIBA).
- ASA/NSAIDs are relatively contraindicated in PwIBD population due to the bleeding disorder.
Refer to your local drug monographs and consider the following: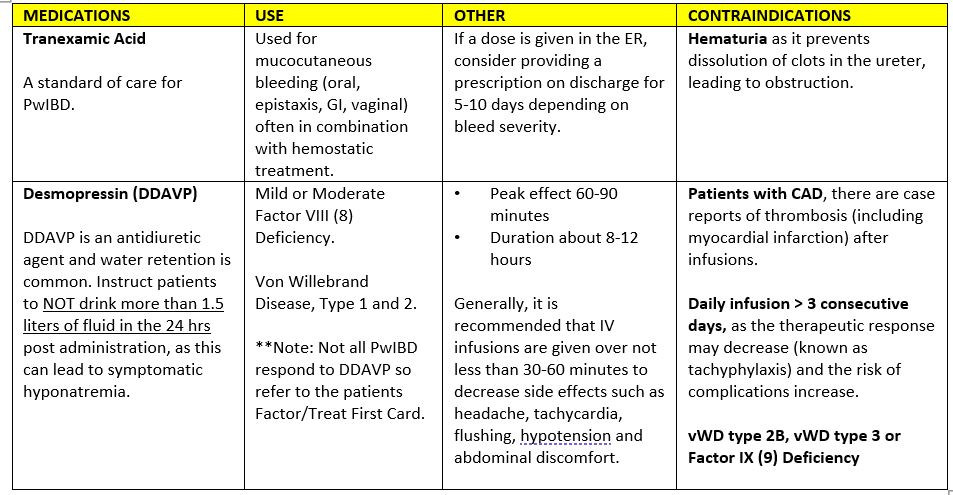
Diagnostic Process
- TREAT FIRST > INVESTIGATE LATER. For a PwIBD it is recommended that treatment should be given BEFORE any diagnostics studies (i.e.: X-rays, CT scans etc) are performed.
- AVOID UNNEEDED PROCEDURES however, for a PwIBD who has an illness that requires an invasive procedure ensure the patient has had appropriate factor/hemostatic treatment BEFORE starting the procedure. Also, consider traumatic repeated venipunctures may cause painful hematomas and limit further IV access.
- AVOID UNNEEDED FACTOR LEVELS. For PwIBD followed by a BC Bleeding Disorder Program, there is no need to order factor levels during the initial admission as their known baseline clotting factor levels, generally remain constant throughout that person’s life.
- AVOID SCREENING ASSAYS In some cases, these assays (i.e.: aPTT, one stage factor levels) will NOT be accurate/reliable depending on the prophylaxis product (i.e.: Emicizumab, Rebinyn) the PwIBD is infusion at home.
- AVOID INTRAMUSCULAR INJECTIONS. If the PwIBD must be given an IM injection, check if hemostatic treatment is required before the injection.
If the patient has NEVER been seen by a hematologist or one of the BC programs, a hematology consult should be completed promptly, and the patient referred to the age-appropriate program. Consider completing a bleeding history, The International Society on Thrombosis and Hemostasis Bleeding Assessment Tool may be used to guide questioning.5
Recommended Treatment
Emergency care of PwIBD sustaining an injury/bleed should include consideration that there could be insidious bleeding.
SOURCES for treatment recommendations:
ASK If they have a Factor/Treat First Card if the patient reports or is known to be a PwIBD. The treatment card provides patient specific dosing for minor/major bleeds and contact information for the appropriate bleeding disorders program. In Hospital Care of Persons with Inherited Bleeding Disorders (PwIBD)
CALL The age-appropriate program immediately. Many PwIBD are followed by the provincial Inherited Bleeding Disorder Programs for their entire lives, and they can provide recommendations.
- Adult Program: P: 604.806.8855 extension 1. After hours, weekends, stats call hematology on call at St Paul’s Hospital P: 604.682.2344
- Pediatric Program: P: 604.875.2406 extension 5335. After hours, weekends and stats call hematology on call at BC Children’s Hospital. P: 604.875.2161
LOOK Is the patient followed by a BC Bleeding Disorders Program?
Non-Cerner sites/Downtime: Find a “Hematology note” posted to CareConnect this should contain recommendations for major/minor bleed treatments.
Cerner sites: Find the “Special Care Plan” (Factor/Treat First Card) on Cerner PowerChart or FirstNet (ED).
Look for the “Special Care Plan” in the Cerner banner.

To access the document: click “documentation filter” menu (left side) >> search note type(s) “Special Care Plan” >> and ensure date typed in is “all dates”. 
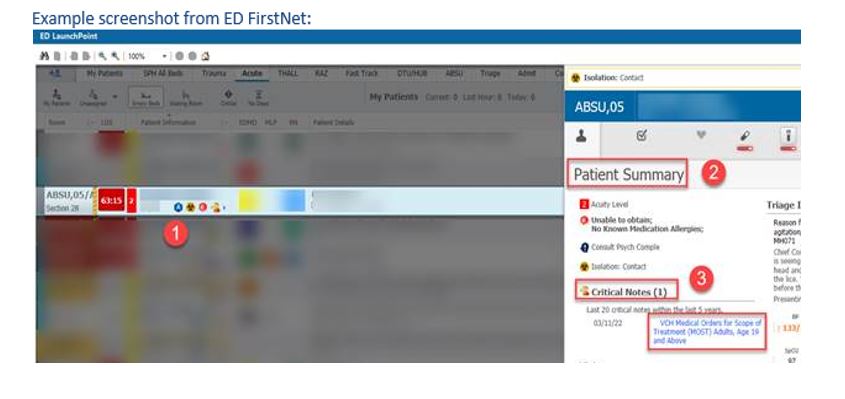
FirstNet (Emergency Departments): Click on the space underneath the patient’s name and “Patient Summary” will display >> Find “Critical Notes” section under Patient Summary>> Click on the Blue Hyperlinks to open up the documented note.
Criteria For Hospital Admission
- Sustained a MAJOR INJURY/BLEED or at risk for compartment syndrome, consider for admission/observation and reimaging.
- Patient is UNABLE TO SELF INFUSE factor products and requires ongoing treatment.
- UNCLEAR PATIENT ABILITY to observe for complications or difficulty establishing a follow-up plan.
Criteria For Transfer To Another Facility
- If major injury/bleed, patient may require transfer to a facility with ICU and 24/7 inpatient hematology support with a coagulation laboratory. For adult patients consider transfer to St Paul’s Hospital or Vancouver General Hospital, for pediatric patients transfer to BC Children’s Hospital (BCCH).
- If a PwIBD requires transportation to another facility for definitive care, all efforts should be made to provide appropriate hemostatic treatment before transport.
Criteria For Close Observation And/or Consult
- Close observation is required if the patient has sustained a major injury/bleed, or at risk for compartment syndrome, and reimaging should be considered.
- If followed by a bleeding disorder program consult the age appropriate program.
- For a new diagnosis consult hematology and refer on to the age appropriate program.
Criteria For Safe Discharge Home
- Reliable and informed patient with means to return if needed.
- Provide clear discharge instructions and discuss a follow-up plan.
- Ensure they have appropriate prescriptions on discharge.
- If followed by a BC Bleeding Disorder Program send an ER discharge summary to the age appropriate program (i.e., ‘SPH Adult Bleeding Disorder Clinic” in VCHA/VIHA Cerner).
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
WFH Guidelines for the Management of Hemophilia and Guidelines on the Diagnosis of von Willebrand Disease, serve as a resource to support education, advocacy, and decision-making related to bleeding disorders treatment and the delivery of care around the world, including developed and underdeveloped countries.
Related Information
If followed by a bleeding disorder program request the patient follows up with the program on discharge. If this is a new diagnosis ensure the age appropriate program referral has been completed & sent, ensure to provide the patient with the clinic contact information.
- Adult Bleeding Disorder Program of BC/Yukon
- P:604.806.8855 ext 1 F:604.806.8784 Email: H&Hclinics@providencehealth.bc.ca
- P:604.682.2344 After hours, w/e and stats call hematology on call at St Paul’s Hospital.
- https://www.providencehealthcare.org/en/clinics/adult-bleeding-disorders-program
- Pediatric Bleeding Disorder Program of BC/Yukon
- P:604.875.2406 F:604.875.2911 Email: hemophilia_clinic@cw.bc.ca
- P:604.875.2161 After hours, w/e and stats call hematology on call at BC Children’s Hospital (BCCH)
- http://www.bcchildrens.ca/our-services/clinics/cancer-blood-disorders/inherited-bleeding-disorders
Further resources:
- Learning Hub: Inherited Blood Disorders. Course code #30138
- Canadian Hemophilia Society: https://www.hemophilia.ca/
- World Federation of Hemophilia: https://wfh.org/about-bleeding-disorders/
- A patient guide to help self administer DDAVP in the context of a bleeding disorder: https://precare.ca/healthcare-guides/ddavp/
Related Information
Reference List
Srivastava A, Santagostino E, Dougall A, et al. WFH Guidelines for the Management of Hemophilia, 3rd ed. Haemophilia. 2020;26(Suppl 6): 1-158. Available from https://onlinelibrary.wiley.com/doi/10.1111/hae.14046
James P, Connell N, Ameer B, et al. ASH ISTH NHF WFH 2021 guidelines on the diagnosis of von Willebrand Disease. Blood Advances. 2021;5 (1): 280-300. Available from https://doi.org/10.1182/bloodadvances.2020003265
Bullard MJ, Chan T, Brayman C, et al. Members of the CTAS National Working Group. Revisions to the Canadian Emergency Department Triage and Acuity Scale (CTAS) Guidelines. CJEM. 2014 Nov.16(6):485-9. PMID: 25358280.
Canadian Hemophilia Society. Emergency Care. Canadian Hemophilia Society. Accessed May 19 2023. https://www.hemophilia.ca/emergency
Rodeghiero F, Tosetto A, Abshire T, et al. ISTH/SSC joint VWF and Perinatal/Pediatric Hemostasis Subcommittees Working Group. ISTH/SSC bleeding assessment tool: a standardized questionnaire and a proposal for a new bleeding score for inherited bleeding disorders. J Thromb Haemost. 2010 Sep;8(9):2063-5. doi: 10.1111/j.1538-7836.2010.03975.x. PMID: 20626619. ISTH-SSC Bleeding Assessment Tool for healthcare providers: Available from https://bleedingscore.certe.nl/
RESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated May 29, 2024
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.