Rapid Change
COVID-19 has rapidly accelerated the use of telehealth or virtual care (VC). However, it is vital that we carefully examine the quality of care being delivered and determine when it is appropriate to use VC as an alternative to face-to-face care. My colleagues and I recently published an article, Principle-driven virtual care practice to ensure quality and accessibility, summarized below, highlighting ways to ensure that VC is used appropriately and ethically for the right health conditions and in the right contexts.
These principles can guide the future VC evolution toward high-quality best practices that also support convenience and equity of access. I welcome your feedback – please comment below!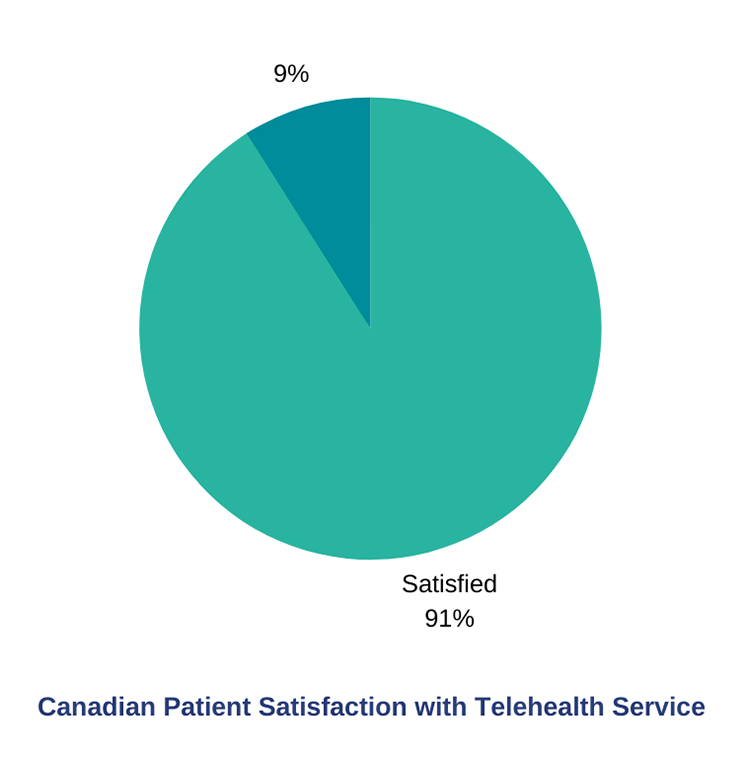
COVID-19 has precipitated a rapid increase in telehealth use. Almost half of all Canadians have now accessed a physician using virtual care options,” with a 91% satisfaction rate among those who experienced this service (source). The need for ongoing VC is clear as the second wave of COVID is upon us.
4 Key Principles
Virtual care should be seen as part of comprehensive care of patients, and the choice of virtual care should benefit our patients and do no harm — a fundamental tenet of medical practice.
There are four key principles to consider to ensure that VC is used appropriately and ethically:
1. Clinical
2. Medicolegal
3. Andragogic
4. Social
Clinical Principles
Clinical quality optimization considerations
- likelihood of accessing in-person care (e.g., patient is in a rural location where timely in-person care is impossible)
- quality, quantity, and reliability of information acquisition
- sufficiency of peripheral observations of the patient
- absence of direct physical examination for clinical decision-making and, in some instances, for meeting the standard of care
- potential of VC to impair judgement or introduce bias in decision-making
- incorporation of current best practices and accepted standard of care in VC
Communication facilitation considerations
- optimizing accuracy in history taking
- sharing of diagnosis and management details with patients
- building a relationship of trust with patients and families
Continuity of care considerations
- establishing a clear process for patient follow up after the VC encounter
- arranging clinical handover of patient information to other health professionals after the VC session, e.g., rural-urban health professional handovers or interprofessional handovers in team-based care
Medicolegal Principles
Informed consent considerations
- proper risk disclosure, frank discussion with patients, and opportunities for them to ask questions
- documentation of informed consent
Confidentiality and privacy considerations
- ensuring the use of secure software and communication infrastructure during patient–physician exchanges
- storing information and preventing unauthorized access by third parties
- maintaining a proper VC record and its availability to patients and caregivers and for medical auditing
Consistency with the legal/regulatory frameworks considerations
- jurisdiction of practice and licensing
- existing telemedicine/VC professional practice guidelines
- privacy and confidentiality guidelines and recommendations
- maintenance and retention of a proper medical record
Transparency of VC involvement considerations
- clear expectations about response times and “when the virtual office is open”
- licensure mechanisms to facilitate the process
- medicolegal protection
- clinical boundaries of acceptable VC care
- service reimbursement
- choosing appropriate software or infrastructure for appropriate VC use by the health system, health professionals, or patients with full understanding of the implications
Andragogic Principles
- Competency-based training
- Harmonization with curricular priorities
- Life-long learning commitment
Social Principles
- Contextual sensitivity versus universality
- Return on investment for all stakeholders
- Social reform and continuous quality improvement
For more details and references, view the full article, Principle-driven virtual care practice to ensure quality and accessibility, in the Canadian Journal of Physician Leadership.
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.